Do you have problems with teeth, gums or oral mucosa?
lege artis products help patients and dentists to overcome problems with:

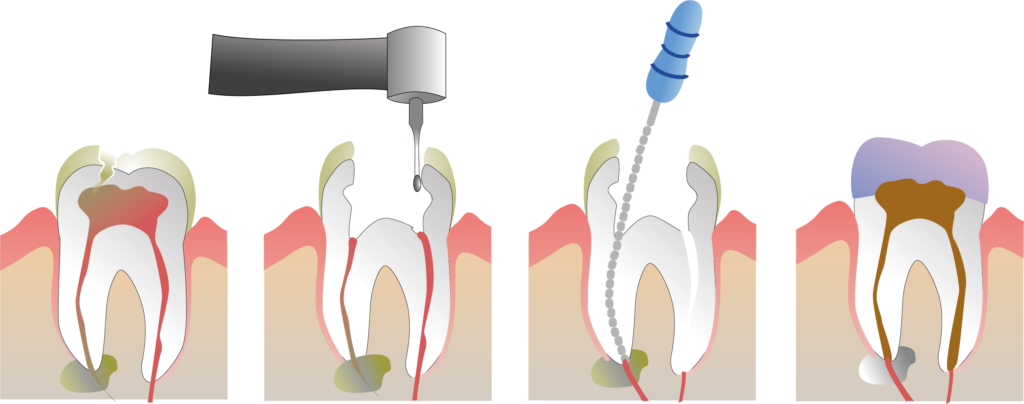
Inflammation of the dental pulp (pulpitis) sometimes causes extreme pain and should therefore be treated by your dentist.
If the inflammation is at an advanced stage and the dental pulp (pulpa) cannot be conserved it has to be removed.
Root treatment involves removing the dental pulp under local anaesthetic, cleaning and disinfecting of the root canal as well as using a filling material with the best possible sealing and wall-permanent properties.
Although the tooth is no more vital after root treatment, it can be conserved and continues to maintain its function.
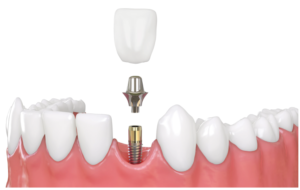
Peri-implantitis is the term for an inflammation around a dental implant, i.e. for pathological changes of the tissue surrounding the implant.
Depending on the severity and nature of thE inflammation, peri-implantitis is sub-classified as:
Peri-implant mucositis
The soft tissue surrounding the implant becomes inflamed, as in gingivitis. It is usually reversible, i.e. it can subside without further sequelae.
Marginal peri-implantitis
If peri-implant mucositis is not treated in time, progressive bone loss also occurs, in a process similar to that seen in parodontitis, which is usually not or only slightly reversible. Marginal peri-implantitis is therefore generally not reversible and can only under certain circumstances be brought under control by surgery.
Retrograde peri-implantitis
This is a special case which only occurs rarely. It is due to residual scar and granulation tissue. As a rule it can be well controlled by curettage of the affected area.
There are some important differences in the structure of the tissue in the mucosa surrounding the implant, some of which can be seen in the opposite figure.
In the connective tissue surrounding the tooth bundles of collagen fibres radiate out into the cement layer of the root of the tooth.
With implants this is not possible. Here the fibre bundles simply run parallel to the surface of the implant.
There are also differences in the composition of the connective tissue. With its high collagen content the connective tissue of the mucosa around the implant is more similar to scar tissue and thus contains distinctly fewer blood vessels. This leads to a fall in immune status and thus to an increase in susceptibility to peri-implant infections.
All peri-implant infections have one thing in common: if they are not treated they lead to loss of the implant. The main causes are bacteria already known from periodontology: Actinobacillus actinomycetemcomitans, Porphyromonas gingivalis, Tannerella forsythensis, Peptostreptococcus micros and Fusobacterium nucleatum.
The biological weak point of all implants is the transition between the oral cavity and the jaw bone at the neck of the implant. The implants available to date have not had this closure, which in natural teeth is impermeable to bacteria.
This area around the implant therefore needs to be particularly thoroughly cleansed and cared for to prevent inflammations developing due to invading bacteria.
In addition to obtaining support from your dentist in the form of dental examinations, instruction in oral hygiene and motivation, checks on the prostheses and, to begin with, annual follow-up x-rays, there are a number of things that you can do to promote long-term success:
Cleansing of implants
It is important to remove plaque and dental calculus thoroughly. This can be done by cleaning the teeth regularly, using dental floss and special brushes and also, where necessary, additional professional cleaning every 6–12 months.
Implant care
The gums surrounding implants should also be cleansed gently and regularly in order to maintain their protective function as effectively as possible.
Using durimplant
The allantoin contained in durimplant soothes and cares for the mucosa and accelerates cell regeneration. The liquid paraffin also cares for the skin and ensures that durimplant is less rapidly removed by the saliva. Sage oil soothes any inflammations before they have the chance to develop further. Thymol, a component of thyme, has a strong disinfectant effect and thus slows bacterial recolonisation.
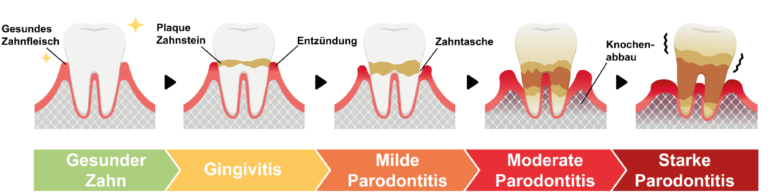
Periodontitis, formerly also known as periodontosis, is an inflammation of the periodontium.
The periodontium itself exists of the jawbone, connective tissue and the gums.
Reddened and inflamed gums and a more frequent occurrence of gum bleeding are indications of a periodontitis.
Regular check-ups at the dentist help to avoid the progress of a not yet identified periodontitis. The dentist can ascertain a periodontitis, inter alia, by screening the gums and measurement of the depth of gingival pockets.
Periodontitis is caused by specific bacteria in the mouth.
Stress or other factors often unbalance our immune system. Then we are especially susceptible to these bacteria which settle on our dental plaque and cause a gingivitis (gum inflammation) by segregation of metabolic products like acids and toxins (poisonous substances).
In the further course gingival pockets, in which bacteria can settle again, occur. The gums regress, the tooth necks are exposed and the bone is attacked.
Several circumstances increase the risk for periodontitis. These include, for example, stress, smoking, diabetes, tartar and insufficient oral hygiene.
Very important is a good oral hygiene:
If you already had a treatment of periodontitis or if you are particularly endangered, we additionally recommend using parodur Gel once a week until once a day, most suitable after the evening teeth brushing. parodur Gel adheres excellent to gums and oral mucosa and therefore it takes an protective and caring effect.
parodur Gel is available in 2 different flavors:
Lime (PZN-09735476) und
Mint (PZN-09735482) in Ihrer Apotheke.
For further treatment and for completion of your personal oral care we recommend parodur Liquid, a soft ready to use mouth rinsing solution which should be applied 1-2x daily and which additionally supports the caries prophylaxis.
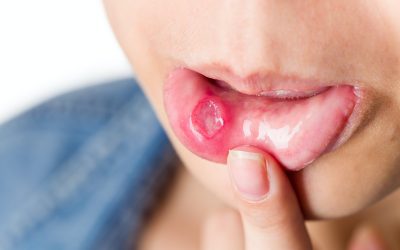

The most frequent diseases of the mouth are recurrent aphthae. These are painful round or oval mucosa defects no bigger than the size of a lentil.
According to modern medical knowledge, these aphthae are neither caused by viruses nor bacteria. Injuries, psychosomatic and hormonal factors, and diet are apparently contributory factors, at least for some patients. As the cause is not certain, it is necessary to apply symptomatic therapy in order to relieve the patient of pain and to shorten the duration of the disease.
LEGASED natur, a viscous, film-forming liquid applied as a protective film in case of aphthae and minor infections in the oral cavity, protects against mechanical pressure and chemical irritation and therefore relieves existing pain.
© Copyright 2021 lege artis Pharma GmbH + Co. KG | All rights reserved | Webdesign by Systeamhaus